Chlamydia often has no warning signs, but untreated infections can cause lasting reproductive health issues. Here’s how to protect yourself and when to get tested.
Chlamydia is the most common STI in South Australia – but most people who have it don’t even know.
That’s partly because it doesn’t usually cause symptoms – and partly because it gets talked about like it’s no big deal. It’s often described as “easy to treat”, so it’s easy to think of it as something annoying but harmless.
And the truth is, chlamydia is easy to treat – especially when it’s caught early, with a test that’s just as simple.
The problem is that when it goes undetected, it can cause serious long-term health issues in some people. And because most people feel completely fine, a lot of infections are picked up late – or not at all.
We asked a sexual health doctor to break down what you actually need to know about this “silent” STI – including how it spreads, how to stay safe, and what can happen if it goes untreated.

What chlamydia actually is – and who it affects
Chlamydia is a bacterial sexually transmitted infection, and it’s the most commonly reported STI in Australia. More than 100,000 cases are diagnosed nationally each year, including thousands in South Australia alone.
Most diagnoses are in people aged 20–29, which makes sense – that’s when a lot of people are dating, hooking up, or getting tested for the first time.
In reality, though, chlamydia is also common in people in their 30s and 40s, and can affect anyone who’s sexually active – whether you’re single, partnered, casually dating, newly divorced, or back on the apps after a long relationship.
“One of the biggest misconceptions is that chlamydia is just a ‘young person’s STI’,” says SHINE SA Sexual Health Doctor and Medical Lead – Education and Advocacy, Dr Clare Keogh. “We see it across all adult age groups.”
Why most people don’t know they have it
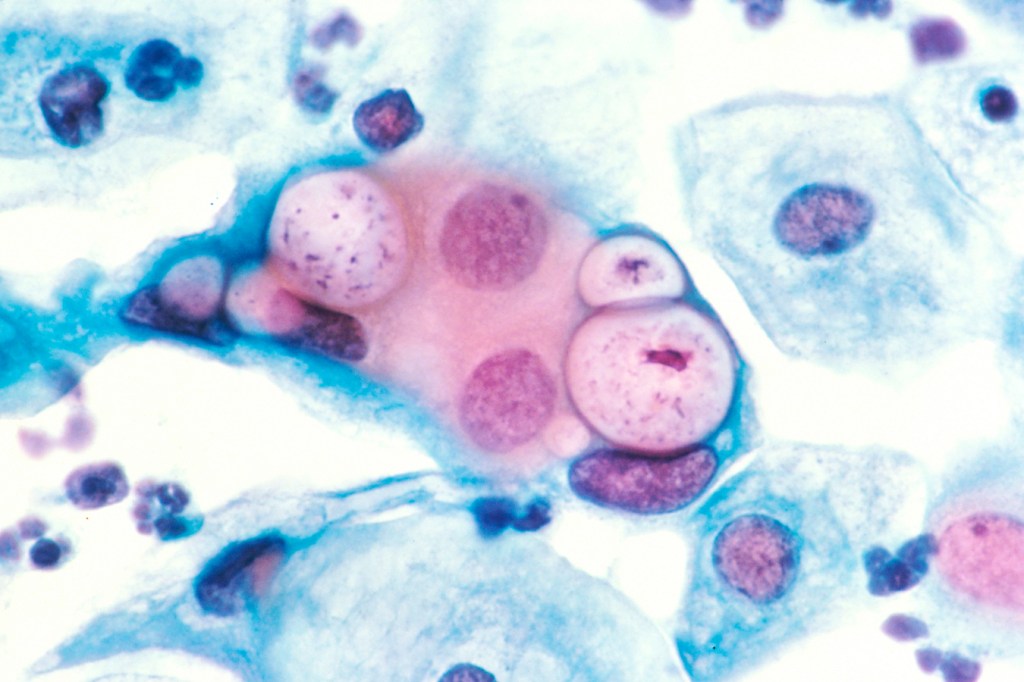
Chlamydia is often described as a “silent” infection – and that’s not an exaggeration.
“More than 80 per cent of people with chlamydia don’t have any symptoms at all,” Dr Clare says. “That’s how it spreads so easily – people don’t realise they have it.”
When nothing hurts and nothing feels wrong, there’s no obvious trigger to get tested. But feeling fine doesn’t mean you’re not infected.
How chlamydia spreads – and why it’s so easy to catch
One of the reasons chlamydia is misunderstood is that not all STIs spread the same way.
Chlamydia spreads through sexual fluids and direct contact with infected mucosal areas.
Mucosa are the soft, moist linings inside parts of the body – including the vagina, penis, anus, mouth and throat.
Because chlamydia infects these areas:
- It doesn’t require ejaculation to spread
- It doesn’t require symptoms
- And it can be passed on even when sexual activity feels low risk
That’s different from:
- Viral STIs like herpes or HPV, which spread through intimate skin-to-skin contact during sex rather than fluids
- Blood-borne STIs like HIV or hepatitis, which are spread through blood and certain body fluids
Understanding this helps explain why chlamydia can be transmitted in intimate situations people don’t always think of as risky – and why condoms really matter.

Symptoms – when they do show up
Most people won’t notice anything at all. But when symptoms do happen, they can include:
- Pain or burning when urinating
- Genital discharge
- Pain in the lower abdomen or pelvis
- Pain or swelling in the testicles
- Bleeding during or after sex
- Bleeding between periods
- Pain, discharge or bleeding from the anus
“The tricky thing is that these symptoms can be mild, vague, or look like something else,” Dr Clare says. “They’re easy to dismiss or brush off.”
Why testing matters – even when nothing feels wrong
Because chlamydia is so often symptom-free, testing is the only real way to know if you have it.
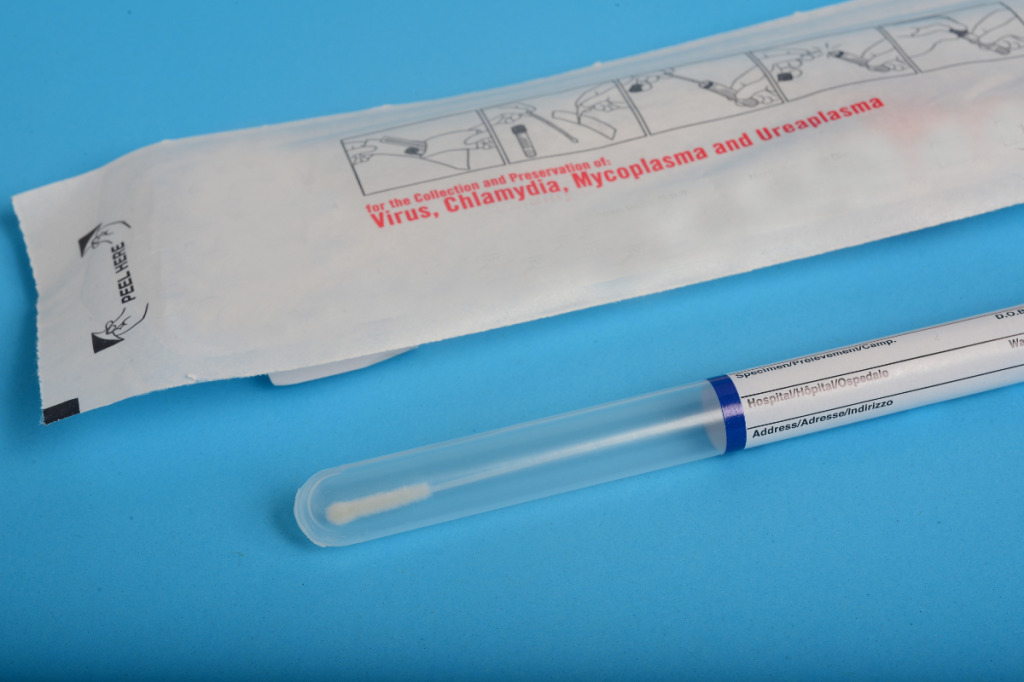
Testing is straightforward and usually involves:
- Peeing in a cup, or
- Doing a self-collected swab
You don’t need to feel unwell to ask for a test. It’s a good idea to get tested if:
- You’ve had a new or changed sexual partner
- You have more than one partner
- You or a partner have symptoms or an STI diagnosis
- You’re under 30 and sexually active, or
- You’re pregnant
“If you’re ever unsure, it’s okay to ask for a test – even if you’re seeing your GP for something completely unrelated,” Dr Clare says.
If you’re not comfortable talking to your GP about STIs, you can make an appointment at your closest SHINE SA clinic. Their nurses provide STI testing free if you’re 21 or under, a full-time student or concession card holder – and the cost is just $35 for everyone else.
If you’re sexually active, Dr Clare says STI testing at least once a year should be a regular part of your healthcare – right up there with visiting the dentist for a check and clean.
And when you ask for an STI test, you’re not just being checked for chlamydia.
The same swab or urine sample is routinely tested for gonorrhoea as well, and your GP will usually recommend adding a simple blood test to screen for syphilis and HIV at the same time.
“Syphilis is increasing among South Australians, and we are sadly seeing cases in babies,” she says. “It’s another one of those infections that can stay hidden for a long time and carry serious risks – so it’s really important to get tested.”
Treatment, reinfection – and why timing matters
Chlamydia is treated with a short course of antibiotics.
During treatment, it’s important not to have sex for seven days, and not to have sex with recent partners until they’ve also completed treatment. That’s how you stop the infection bouncing back and forth.
Reinfection is common, which is why people who test positive are advised to have another test three months later.
“If chlamydia is picked up early and treated, most people won’t have any long-term problems,” Dr Clare says. “The issues arise when it goes undetected.”
This is especially important during pregnancy. If chlamydia isn’t picked up and treated, it can increase the risk of pregnancy complications and, in some cases, be passed on to a baby during birth, causing infections in the eyes or lungs. Testing is simple and treatment is safe during pregnancy, which is why early screening and follow-up testing matter.
The long-term risks – including infertility
This is the part people often don’t realise. Untreated chlamydia can spread to the reproductive organs and cause serious complications – even when there are no obvious warning signs.
In people with a uterus, it can lead to pelvic inflammatory disease, which may cause chronic pelvic pain, ectopic pregnancy and infertility.
In people with testicles, it can cause epididymo-orchitis – an infection that can lead to pain and swelling in the scrotum, and may also affect fertility.
What makes this worse is that chlamydia can do this kind of internal damage quietly, with little or no symptoms at all. Many people only find out years later, when they’re trying to have kids – or simply trying to keep their options open.
“Infertility isn’t inevitable,” Dr Clare says. “But the risk increases when infections aren’t picked up and treated.”

How to reduce your risk (yes – condoms)
Condoms are one of the most effective ways to reduce the risk of chlamydia.
Because chlamydia spreads through mucosal contact and sexual fluids, condoms create a physical barrier that significantly lowers the chance of transmission – especially with new or casual partners.
Condoms work best alongside regular testing, not instead of it.
“Condoms and testing together are what really protect your sexual health,” Dr Clare says.
There are also additional prevention options for people at higher risk of STIs.
One of these is a medication taken after sex called Doxy-PEP. It’s primarily used to reduce the risk of syphilis, but it can also lower the chance of developing chlamydia and gonorrhoea.
“It’s like the emergency contraceptive – the morning after pill – but for syphilis and other STIs,” Dr Clare says.
Doxy-PEP is an extra layer of protection – not a substitute for condoms or regular testing. If you think you might be at higher risk, speak with your GP or the clinicians at SHINE SA about whether it’s appropriate for you.

Telling partners – without awkward conversations
If you test positive, letting recent sexual partners know is important so they can get tested and treated too. That helps prevent reinfection and stops the infection circulating.
If the idea of that conversation makes you want to crawl into a hole, you’re not alone – and you don’t have to do it face-to-face.
There are anonymous notification services that can send a simple text message for you, including:
“These tools take a lot of the stress out of it,” Dr Clare says. “They help people do the right thing without putting themselves in uncomfortable or unsafe situations.”
Still have questions?
SHINE SA offers:
- A free and confidential sexual healthline: 1300 883 793, Monday-Friday, 9am-12:30pm.
- Handy factsheets (start here) and resources on their website.
- Friendly, inclusive clinics where awkward questions are welcome.

















